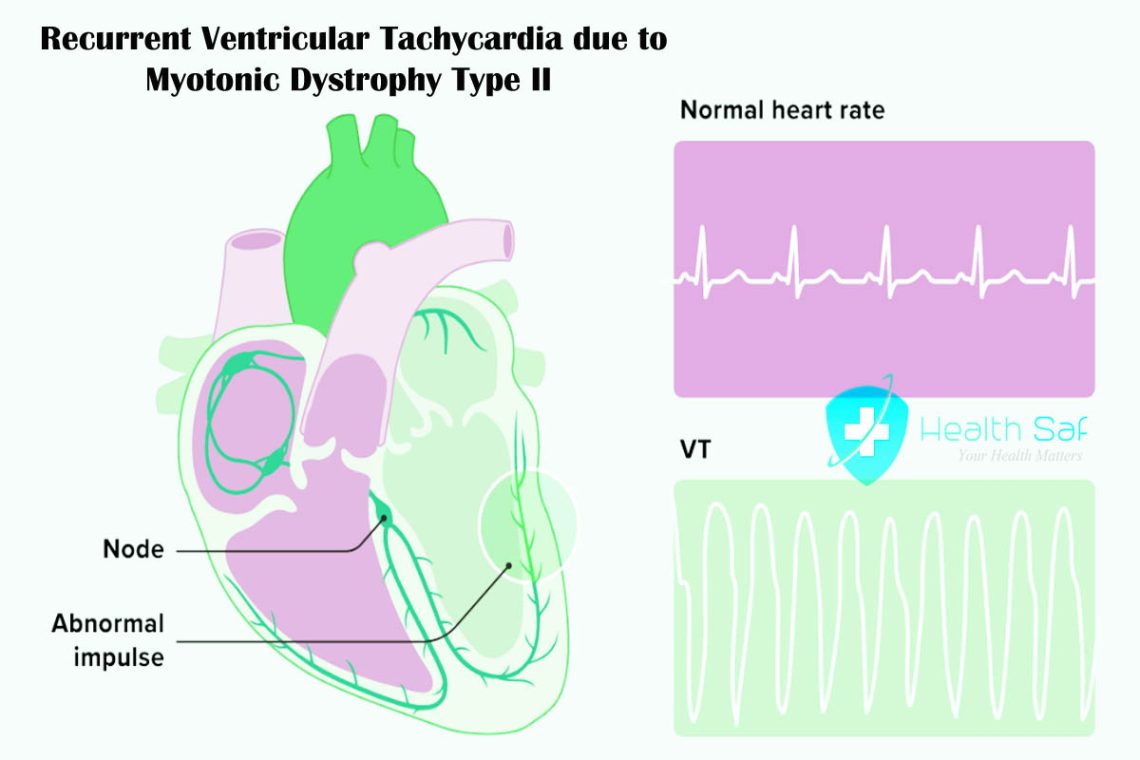
Learn what recurrent ventricular tachycardia due to myotonic dystrophy type II is and how it can affect a person. This guide discusses the diagnosis, causes, and treatments for those suffering with this condition.
Recurrent ventricular tachycardia due to myotonic dystrophy type II is a rare medical condition involving abnormal electrical signals in the heart. People living with this condition may experience symptoms such as palpitations, dizziness, and shortness of breath. In this guide, you will find information on its diagnosis, causes, and treatments to consider.
Table of Contents
Myotonic Dystrophy Dilated Cardiomyopathy
Recurrent ventricular tachycardia due to myotonic dystrophy type II is a rare medical condition that occurs when an individual’s electrical circuitry in the heart begins to malfunction. The condition usually appears with little warning and often leads to bouts of palpitations, dizziness, or shortness of breath. To reduce the risk for this condition, diagnosis can be made through specialized imaging equipment and tests. Furthermore, there are specific treatments available which may help reduce the severity of episodes or even eliminate them entirely.
What Causes Recurrent Ventricular Tachycardia in Myotonic Dystrophy Type II?

Recurrent ventricular tachycardia due to myotonic dystrophy type II is caused by a genetic mutation that disrupts the proper functioning of the heart. This mutation can cause the electrical circuitry of the myocardium—the muscle layer surrounding the heart—to malfunction, causing sudden arrhythmia or a condition known as tachycardia. Tachycardia causes an excessive and dangerous heart rate of more than 100 beats per minute, which can lead to adverse symptoms including chest pain, lightheadedness, and fainting.
What is the Best Treatment for Ventricular Tachycardia?
Recurrent ventricular tachycardia due to myotonic dystrophy type II is usually diagnosed through a physical examination, laboratory tests, and an electrocardiogram. An electrocardiogram (ECG) is used to detect abnormal heart rhythms and other tell-tale signs of the condition. Other diagnostic tools may also be used such as an echocardiogram, stress test, or a Holter monitor, which is worn for 24 hours to measure your heart rhythm over time.
How is Recurrent Ventricular Tachycardia Treated in Myotonic Dystrophy Type II?
Treatment of recurrent ventricular tachycardia due to myotonic dystrophy type II may include medications, ablation therapy, and implantable devices. Medications such as beta blockers or calcium channel blockers may be given to help control heart rate or rhythm. Ablation is a procedure that can help remove the abnormal areas of tissue that are causing unproductive electrical signals from occurring within the heart. Finally, there are implantable devises available, such as an implantable cardioverter defibrillator (ICD), which allow your doctor to monitor your heart rhythm and deliver therapies if needed.
What Complications Might be Associated with Recurrent Ventricular Tachycardia Due To Myotonic Dystrophy Type II?

Recurrent ventricular tachycardia due to myotonic dystrophy type II can have serious complications due to an arrhythmia. These complications may include an increased risk of stroke, heart failure, cardiac arrest, and death. It is important for those with myotonic dystrophy type II to visit their doctor regularly in order to monitor the recurrent ventricular tachycardia and prevent any potential long-term consequences.
Myotonic Dystrophy Cardiomyopathy
Myotonic dystrophy (DM) is a genetic disorder that affects multiple systems in the body, including the muscles and the heart. The Myotonic dystrophy cardiomyopathy (DM-CM) is a specific type of heart muscle disease that occurs in some individuals with DM.
DM-CM is characterized by a weakening of the heart muscle, which can lead to problems such as heart failure and abnormal heart rhythms. Symptoms of DM-CM can include shortness of breath, fatigue, and chest pain. In severe cases, it can also lead to heart attack or sudden death.
The exact cause of DM-CM is not fully understood, but it is thought to be related to the genetic mutations that cause DM. The condition is caused by expansion of a CTG repeat in the DMPK gene which leads to abnormal protein accumulation in various tissues including heart muscle.
Treatment for DM-CM typically involves managing the symptoms and complications of heart failure, such as with medications, lifestyle changes, and in some cases, surgery or other medical procedures.
Conclusion
Individuals with DM should be closely monitored for the development of heart problems, including DM-CM. This typically involves regular monitoring of heart function through tests such as electrocardiograms (ECGs) and echocardiograms (ultrasound of the heart).
Also Read: What is the use of Monatomic Gold?